Events Info
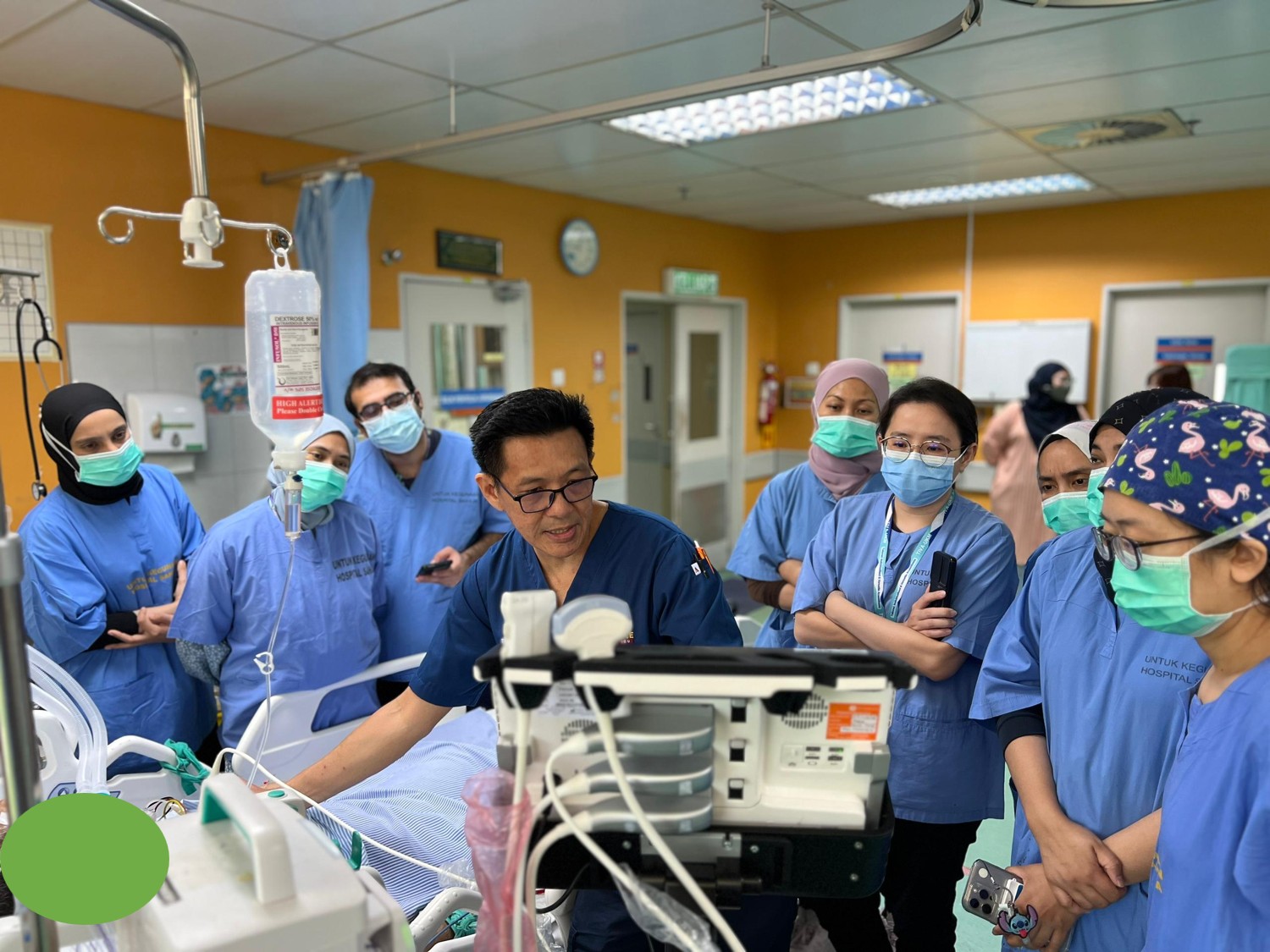
PICU Masterclass Series
Various Date
LOTUS SUNMED CONVENTION CENTRE
Sunway Medical Centre, Sunway City
Basic Assessment and Support In Intensive Care
5-6 November 2025
Hospital Sungai Buloh, Selangor
Intensive Care Nephrology Beyond BASIC
26 & 27 November 2025
Medical Academies Building, Precinct 8, Putrajaya